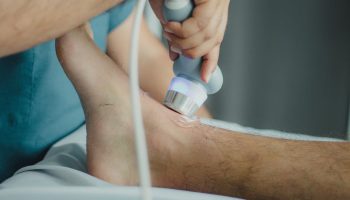
Recent scientific discoveries are reshaping our understanding of chronic back pain, particularly how our bodies naturally regulate pain signals. Scientists have identified a hormone that may hold the key to stopping chronic back pain at its biological source, offering hope for millions of desk workers and others suffering from persistent spinal discomfort.
📑 Table of Contents (click to collapse)
- Key Takeaways
- The Hormone Discovery: A New Hope for Chronic Pain
- Pain Reprocessing Therapy: Retraining Your Brain's Response
- The Surprising Connection: Back Pain and Sound Sensitivity
- Integrating New Science with Practical Solutions
- The Future of Back Pain Treatment
- Practical Steps You Can Take Today
-
Frequently Asked Questions
- Can this newly discovered hormone actually cure my chronic back pain from sitting at my desk all day?
- How does Pain Reprocessing Therapy actually work for someone with desk-related back pain?
- Why does my back pain seem worse in noisy office environments?
- Should I still focus on ergonomics and posture if chronic back pain is really about brain processing?
- What can I start doing today to address the neurobiological aspects of my chronic back pain?
- Conclusion: A New Era of Back Pain Understanding
This breakthrough research, combined with emerging findings about pain processing therapy and the complex relationship between our brains and chronic pain, suggests we’re entering a new era of back pain treatment that focuses on root causes rather than temporary symptom relief.
Key Takeaways
- Scientists have discovered a hormone that may naturally regulate chronic pain signals in the spine
- Pain Reprocessing Therapy shows long-term effectiveness for chronic back pain, addressing brain-based pain mechanisms
- Understanding the neurobiological basis of chronic pain opens new treatment pathways beyond traditional approaches
- Desk workers can benefit from therapies that retrain how the brain processes pain signals
- The discovery highlights the importance of treating chronic pain as a neurological condition, not just a structural problem
The Hormone Discovery: A New Hope for Chronic Pain
According to recent research published by scientists, a newly identified hormone appears to play a crucial role in regulating chronic pain signals within the spinal cord. This discovery represents a significant shift from traditional approaches that focus primarily on structural issues like herniated discs or muscle tension.
The hormone works by modulating how pain signals are transmitted from the spine to the brain, potentially offering a biological “off switch” for chronic pain conditions. For desk workers who develop persistent back pain from prolonged sitting and poor ergonomics, this could mean addressing the underlying neurobiological mechanisms rather than relying solely on ergonomic adjustments and pain medications.
What makes this discovery particularly significant is that it addresses chronic pain at the cellular level. Unlike acute pain, which serves as a protective warning system, chronic back pain often persists long after any initial injury has healed. This hormone may help explain why some people develop chronic pain while others recover completely from similar injuries.
Pain Reprocessing Therapy: Retraining Your Brain’s Response
Complementing the hormone discovery, research from the University of Colorado Anschutz demonstrates that Pain Reprocessing Therapy (PRT) provides long-term relief for chronic back pain. This therapy works by helping the brain reinterpret pain signals, essentially “retraining” neural pathways that have become hypersensitive to normal sensations.
For desk workers experiencing chronic back pain, PRT offers a drug-free approach that addresses the neurological aspects of persistent pain. The therapy teaches patients to recognize when their brain is creating or amplifying pain signals unnecessarily, providing tools to break the cycle of chronic discomfort.
How PRT Works for Desk Workers
Pain Reprocessing Therapy operates on the principle that chronic pain often involves the brain misinterpreting safe signals as dangerous. For someone who spends hours at a desk, normal sensations from sitting or minor muscle tension can be amplified into significant pain through learned neural patterns.
- Somatic Tracking: Learning to observe physical sensations without fear or catastrophic thinking
- Cognitive Restructuring: Identifying and changing thoughts that amplify pain perception
- Graduated Exposure: Gradually returning to activities that have been avoided due to pain fears
- Pain Education: Understanding the neuroscience behind chronic pain to reduce fear and anxiety
The Surprising Connection: Back Pain and Sound Sensitivity
Recent research has also uncovered an unexpected link between chronic back pain and sensitivity to loud noises. This finding, reported by The Washington Post, suggests that chronic pain conditions may involve broader sensory processing changes in the nervous system.
For office workers, this connection has practical implications. Open office environments with high noise levels might not only create stress and concentration difficulties but could also potentially amplify existing back pain conditions. Understanding this relationship helps explain why some people with chronic back pain also experience heightened sensitivity to environmental stimuli.
Managing Sensory Overload in the Workplace
- Use noise-canceling headphones during focused work periods
- Create visual barriers or work in quieter areas when possible
- Practice stress-reduction techniques to lower overall nervous system reactivity
- Consider requesting workplace accommodations if sensory sensitivity affects your pain levels
Integrating New Science with Practical Solutions
While we await the development of hormone-based treatments for chronic back pain, desk workers can immediately benefit from understanding the brain’s role in pain processing. This knowledge shifts focus from purely mechanical solutions to include neurological approaches.
Evidence-Based Strategies for Desk Workers
Mindfulness and Pain Awareness: Developing a non-judgmental awareness of pain sensations can help break the fear-pain cycle. Recent studies suggest that mindfulness meditation can actually change how the brain processes pain signals, similar to the mechanisms involved in PRT.
Movement as Medicine: Regular movement throughout the workday isn’t just about preventing muscle stiffness—it also helps maintain healthy pain processing pathways in the brain. Even brief movement breaks can signal to the nervous system that the body is safe and functioning normally.
Stress Reduction: Since chronic stress can amplify pain signals and potentially interfere with the body’s natural pain-regulating hormones, managing workplace stress becomes a crucial component of back pain prevention and treatment.
The Future of Back Pain Treatment
The hormone discovery represents just the beginning of a new understanding of chronic pain. As researchers continue to unravel the complex interactions between hormones, neural pathways, and pain perception, we can expect more targeted treatments that address the biological roots of persistent pain.
For now, this research validates what many pain specialists have long suspected: chronic back pain is not simply a matter of damaged tissues or poor posture, but a complex neurobiological condition that requires multifaceted treatment approaches.
What This Means for Treatment Decisions
- Consider therapies that address both physical and neurological aspects of pain
- Don’t dismiss pain education and brain-based treatments as “not real medicine”
- Work with healthcare providers who understand the complexity of chronic pain
- Be patient with recovery—retraining neural pathways takes time
Practical Steps You Can Take Today
While we wait for hormone-based treatments to become available, there are evidence-based actions you can take immediately to address the neurobiological aspects of back pain:
- Learn about pain science: Understanding how chronic pain works can reduce fear and anxiety, which often amplify pain signals
- Practice somatic tracking: Spend a few minutes daily observing physical sensations without trying to change them
- Address catastrophic thinking: Challenge thoughts like “my back is getting worse” or “I’ll never get better”
- Gradually increase activity: Don’t let fear of pain prevent you from normal movement and activities
- Consider professional help: Seek out healthcare providers trained in pain reprocessing therapy or similar approaches
Frequently Asked Questions
Can this newly discovered hormone actually cure my chronic back pain from sitting at my desk all day?
While the hormone discovery is promising, treatments based on this research are not yet available to patients. However, the discovery validates that chronic back pain has biological roots beyond just poor posture or damaged tissues. Currently, you can benefit from Pain Reprocessing Therapy and other brain-based approaches that work with your body's existing pain regulation systems while researchers develop hormone-based treatments for the future.
How does Pain Reprocessing Therapy actually work for someone with desk-related back pain?
Pain Reprocessing Therapy teaches your brain to reinterpret pain signals that have become unnecessarily amplified. For desk workers, normal sensations from sitting or minor muscle tension can trigger significant pain through learned neural patterns. PRT uses techniques like somatic tracking, cognitive restructuring, and graduated exposure to help you recognize when your brain is creating unnecessary pain and provides tools to break this cycle.
Why does my back pain seem worse in noisy office environments?
Recent research shows an unexpected connection between chronic back pain and sensitivity to loud noises, suggesting that chronic pain involves broader sensory processing changes in your nervous system. Open office environments with high noise levels can potentially amplify existing back pain conditions by increasing overall nervous system reactivity. Using noise-canceling headphones and creating quieter work spaces may help reduce this amplification effect.
Should I still focus on ergonomics and posture if chronic back pain is really about brain processing?
Yes, but with a broader understanding. While ergonomics and posture remain important for preventing initial injury and maintaining comfort, addressing chronic back pain requires a multifaceted approach that includes both physical and neurological aspects. The new research shows that chronic pain often persists even after tissues heal, so combining good ergonomics with brain-based therapies like pain education and stress reduction provides the most comprehensive approach.
What can I start doing today to address the neurobiological aspects of my chronic back pain?
You can immediately begin learning about pain science to reduce fear and anxiety that amplify pain signals. Practice somatic tracking by spending a few minutes daily observing physical sensations without judgment. Challenge catastrophic thoughts about your pain and gradually increase normal activities without letting fear hold you back. Consider seeking healthcare providers trained in Pain Reprocessing Therapy or similar brain-based approaches to chronic pain.
Conclusion: A New Era of Back Pain Understanding
The discovery of hormones that regulate chronic pain, combined with the proven effectiveness of Pain Reprocessing Therapy, marks a paradigm shift in how we understand and treat persistent back pain. For desk workers who have struggled with chronic discomfort despite ergonomic improvements and traditional treatments, these findings offer genuine hope.
The key insight is that chronic back pain is not just about what’s wrong with your spine—it’s about how your nervous system processes and interprets signals from your body. By addressing both the biological and neurological aspects of pain, we can move beyond merely managing symptoms to actually resolving the underlying condition.
Start by educating yourself about the science of pain, consider brain-based treatment approaches alongside traditional ergonomic solutions, and remember that recovery from chronic pain is not only possible but increasingly achievable with the right understanding and tools. The future of back pain treatment is here, and it’s more hopeful than ever before.
Watch: Exercises for Chronic Lower Back Pain
Video courtesy of AskDoctorJo
Recommended Reading
As an Amazon Associate, we earn from qualifying purchases.
- The Way Out by Alan Gordon ($11.29 from Amazon) — Available in paperback, Kindle, and audiobook
- Explain Pain by Butler & Moseley ($142.78 from Amazon) — Available in paperback, Kindle, and audiobook
- Healing Back Pain by Dr. John Sarno ($10.50 from Amazon) — Available in paperback, Kindle, and audiobook
- The Back Pain Revolution by Gordon Waddell ($105.44 from Amazon) — Available in paperback, Kindle, and audiobook